Scientific Background
Bilateral, permanent, sensorineural hearing loss, with an incidence of 1:500 newborns, is one of the most common congenital disorders. In adults, the prevalence is up to 3.5:1,000. The proportion of genetically caused sensorineural deafness is about 50-70%. Only a small percentage of prelingual deafness is syndromic or has autosomal dominant or mitochondrial inheritance. More than 70% of genetic deafness is non-syndromic, and about 80% of non-syndromic genetic deafness follows an autosomal recessive inheritance. With the investigation of the GJB2 and GJB6 genes, about 50% of the cases of autosomal recessive, non-syndromic, sensorineural deafness can be clarified.
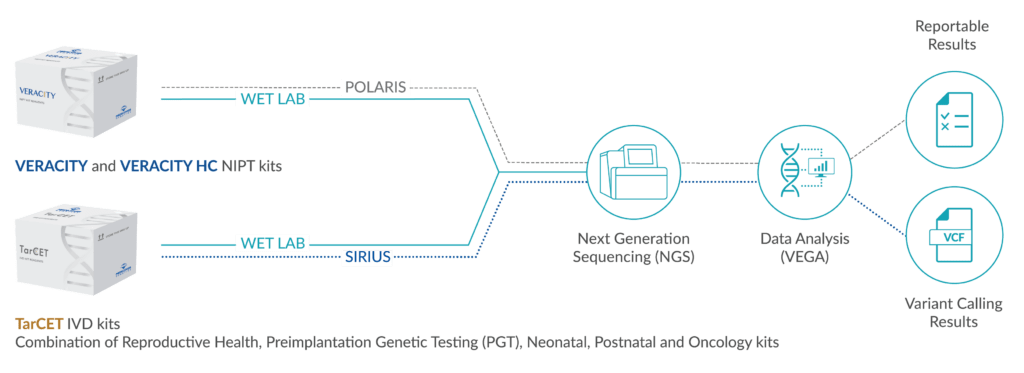
Due to the clinical and genetic heterogeneity of congenital hearing disorders, a step-by-step diagnosis using NGS with the additional analysis of well over 100 genes, including mitochondrially coded ones, may be useful. When requesting these panels, pedigree information and comprehensive clinical data are urgently needed to ensure reliable interpretation.
DEAFNESS/HEARING LOSS, CONGENITAL, SENSORINEURAL
Congenital sensorineural deafness is estimated in the literature to have an incidence of 1-4:1,000. The proportion of sensorineural deafness with a genetic cause is 50%. 70% of genetic deafness is non-syndromic and 30% syndromic. 80% of non-syndromic cases are inherited in an autosomal recessive manner. Pathogenic variants in the GJB2 gene are causative in up to 50% of all autosomal recessive cases of deafness and in up to 35% of sporadic cases. The gene product, connexin 26, is an essential component of gap junctions and thus involved in the formation of cell-cell connections. The most common pathogenic variant in the GJB2 gene, the deletion of a guanine (35delG), leads to the functional loss of one allele, is detectable in about 60-80% of the mutant alleles and occurs in the total population with an allele frequency of about 1%.
Many pathogenic variants of the GJB2 gene are now known and sufficient clinical and genetic data are available to establish a genotype-phenotype correlation. A deletion in the GJB6 gene (gap junction protein connexin 30), del(GJB6-D13S1830), may also be the cause of autosomal recessive non-syndromic deafness, especially in combination with heterozygous GJB2 alterations. In addition, alterations in more than 150 other genes are known that can lead to autosomal recessive or autosomal dominant inherited non-syndromic deafness.
Pathogenic mitochondrial variants can be detected in <1% of patients with prelingual sensorineural hearing loss and 2-27% of postlingual forms. Irreversible hearing loss is a serious complication of treatment with aminoglycoside antibiotics such as streptomycin, gentamycin and kanamycin. Base pair substitutions at positions 1555, 7444, 7445, 7510 and 7511 of the mitochondrial genome are associated with non-syndromic sensorineural hearing loss and an increased risk of aminoglycoside-induced deafness. In contrast to classical Mendelian inheritance, mitochondrial genes are inherited maternally. In addition, further variants of the mitochondrial genome have been described that lead to syndromic or even non-syndromic forms of hearing loss.
References
Del Castillo et Del Castillo 2017, Front Mol Neurosci https://doi. org/10.3389/fnmol.2017.00428 / Chan et Chang 2014, Laryngos 124:E34 / Mani et al. 2009, Eur J of Hum Genet 17:502 / Petersen et al. 2006, Clin Genet 69:371 / Snoeckx et al. 2005, Am J Hum Genet 77:945 / Cryns et al. 2004, J Med Genet 41:147 / Pallares-Ruiz et al. 2002, Eur J Hum Genet 10:72 / Rabionet et al. 2000, Hum Genet 106:40
DEAFNESS/HEARING LOSS, MITOCHONDRIAL (ALSO DRUG-INDUCED)
Irreversible hearing loss is a serious complication of treatment with aminoglycoside antibiotics such as streptomycin, gentamicin and kanamycin. It has been known for many years that pathogenic variants in the maternally inherited mitochondrial (mt) genes play an important role in this. Mt variants at positions m.1494C>T and m.1555A>G of the mitochondrial 12S rRNA gene (MT-RNR1) are associated with the risk of aminoglycoside-induced deafness. Other variants are also listed in the database for mt variants (MITOMAP), although their significance in this context is still unclear. The mechanism of action of the aminoglycosides is based on irreversible binding to the related 30S subunit of the bacterial ribosomes, which leads to a disruption of protein biosynthesis.
The variant m.7445A>G in the MT-TS1 precursor gene, which codes for the mitochondrial tRNASer(UCN) and simultaneously affects the MT-CO1 gene (mitochondrial cytochrome C oxidase subunit 1), has also been identified in connection with aminoglycoside-induced hearing loss, although this variant has also been detected in patients with non-syndromic sensorineural hearing loss without antibiotic use. In addition, other mt variants, such as m.3243A>T and m.3243A>G, have been described in connection with non-syndromic sensorineural hearing loss and their pathogenicity has been confirmed; the latter being the most common mt variant. In Finland m.3243A>G is found in 7.4% of the above mentioned patient group. The variant is associated with a broad phenotypic spectrum, including mitochondrial myopathy, encephalopathy, lactic acidosis and stroke-like episodes (MELAS), maternally inherited diabetes and deafness (MIDD) and chronic progressive external ophthalmoplegia (CPEO).
References
Fujimoto et Yamasoba 2019, Antioxidants 8:109 / Mutai et al. 2017, BMC Medical Genet 18:32 / Pandey & Pandey 2015, dx.doi. org/10.5772/61218 / Bitner-Glindzicz et al. 2009, N Engl J Med 360:640 / Vandebona et al. 2009, N Engl J Med 360:642 / Maász et al. 2008, Curr Med Chem 15:1257 / Jin et al. 2007, Biochem Biophys Res Commun 361:133 / Ballana et al. 2006, Biochem Biophys Res Commun 341:950